This is the last article you can read this month
You can read more article this month
You can read more articles this month
Sorry your limit is up for this month
Reset on:
Please help support the Morning Star by subscribing here
RECENT figures released by The Lancet reveal self-harm is on the rise for both sexes and all age groups.
It has long been recognised this is a huge problem among young people, and as such some services have been set up for this age group, though the provision is patchy.
The authors of the report say the worry is that self-harming behaviour among young people risks becoming “normalised.”
What these Lancet figures also show is there is a need for age and gender-appropriate support. The lack of such provision for those who are older results in many people not seeking help, and for those who do, the only place they can go to is an accident and emergency department (A&E).
Attending an A&E unit for help due to self-harm requires a leap of faith. These patients put their trust in the nursing staff and although some receive good care, a substantial number do not.
Psychiatrist Rosie Claverton said that if staff have a poor attitude towards someone who self-harms it can increase the distress and risks, as it will make them reluctant to seek help in the future.
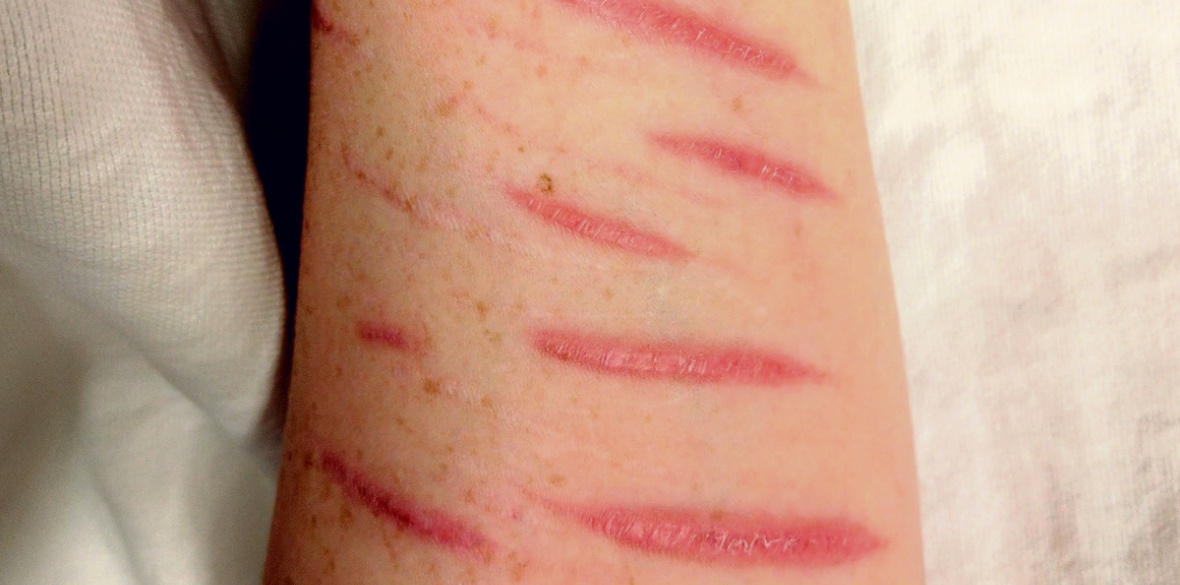
Jane, who was in her early forties, recently had to visit a large London teaching hospital for help with a wound on her arm.
After her wound had been stitched, she was taken to a completely bare room by the nurse: “I was told to lie down,” Jane recalls. “They gave me a blanket — just like being in a prison cell.”
Jane, who is from Brighton but was visiting London for the day, was terrified and wanted to leave. Yet, despite this, she was being detained against her will, though not by any legal means such as being sectioned under the Mental Health Act.
Eventually a nurse came into the room and proceeded to “pat” Jane down, feeling her breasts over her clothes and other areas of her body. She was told to take off her shoes. After that, she was asked to hand over her bag, which was searched in front of her before it was confiscated.
“I felt too shocked to say anything when she was searching me,” Jane said. “It was also humiliating when she went through the contents of my bag. Also, I’m the main contact for my mother. If she can’t get in touch with me, she starts to panic. So, when they confiscated my bag and phone, without any reason why they were doing it, I got very anxious.”
After five hours in A&E Jane was allowed to leave. In this time, she hadn’t eaten, had anything to drink, or been to the toilet. She had been far too scared to ask.
A few weeks after Jane was treated, Mich, 36, from north Wales was taken to an A&E after a large overdose.
As he waited to be seen by a doctor, he developed red spots all over his skin and was feeling weak and confused. He staggered over to where three nurses were talking and told them about it, but instead of examining him, they began questioning him about the overdose in an aggressive manner: “They provoked me, guilt-tripping me, saying how could I do this with a young family.
“Just by them saying that, I knew they didn’t know anything about my situation. I tried to back away, but they carried on prodding me until I got angry.
“Next thing, I was taken into this room where I was told boundaries had to be set because my behaviour towards staff was unacceptable.”
What is behind this poor treatment?
“Burnout and compassion fatigue are increasingly common in the NHS front line,” Claverton says, “but although this might offer an explanation it is not an excuse for these negative, harmful attitudes.”
Jane and Mich both felt some nursing staff still equate self-harm with misinformed and deeply damaging opinions about borderline personality disorder (BPD).
So, instead of a nurse or doctor seeing a patient in genuine distress, they would be viewed as manipulative — using self-harm as a way to get attention.
For these and many other reasons, a BPD diagnosis is contentious, and as such, should not be used as a justification for poor care.
There are many reasons behind self-harm. It isn’t limited to one particular diagnosis or even having a mental illness.
The only certainty are the benefits that both a service user and nurse can receive from a relationship with mutual respect, sensitivity and compassion.
The National Institute for Health and Care Excellence advise that “people who have self-harmed should be treated with the same care, respect and privacy as any patient.
“This is the so-called ‘parity of esteem’ — a concept where mental and physical healthcare should be given equal priority in healthcare delivery.”
But, as Claverton points out: “From funding to practice, we are nowhere near this being achieved — and as a result people who self-harm are being let down.”
Whatever you’re going through you can call Samaritans free of charge on 116 123, any time day or night. Or you can email [email protected].
Some names have been changed to protect their identity.
Rosie Claverton is a psychiatrist and an author (rosieclaverton.com)
Ruth F Hunt is an author and freelance journalist.